Dr. Maranga: Fighting Cervical Cancer with both Prevention and Treatment
30 August 2018 – On the border of Africa’s biggest slum, Kibera, Dr. Orora Maranga sat in his modest women’s health practice and worried aloud about the cervical cancer burden in Kenya. He is a humble, soft-spoken man.
“I see women dying unnecessarily and most of it is because they come late for the consultation,” said Dr. Maranga. “More than 80 percent of women who come here for diagnosis are with some form of advanced cervical cancer.”
Cervical cancer is preventable. Most cases are caused by a very common virus, called human papillomavirus, or HPV. Safe and effective vaccination against HPV can prevent cervical cancer, as can screening women for pre-cancerous lesions, and immediately treating those lesions to stop their progression to cervical cancer.
But despite the existence of these simple, proven prevention tools, cervical cancer is the most frequent cancer among women in Kenya. In 2017 alone, the country registered 4,800 new cases, and approximately 2,450 women lost their lives to the disease. The situation is similar in other low- and middle-income countries. Though Dr. Maranga and others provide cervical screening services, there is still a high cervical cancer mortality rate due a lack of awareness, inadequate access to health care, and patients’ lack of means to afford health services.
According to Dr. Maranga, the Kenyan government should make cervical cancer services “more accessible, more affordable and in a way it should be better if they were actually free to our patients.”
Magdalene Njoki Gachui is a Kenyan mother whose experience is typical of cervical cancer patients who struggle to afford treatment. “I’m the only breadwinner in the family and now I can’t even afford money to come to the hospital,” she said, agonizing about where she would find money “for transport to the hospital, what I’ll eat and where I’ll stay.”
In addition to managing his private practice working as consultant obstetrician, gynecologist and oncologist at Kenyatta National Hospital, Dr. Maranga finds time to run a charity that provides free treatments to cervical cancer patients like Magdalene. At least 1,500 patients have received life-saving services, but such programs need resources to reach the many more women who need them.
“There are organizations on the ground both vaccinating and screening women, but they are doing it on a very small scale. And why is that? Because they don’t have enough funding,” said Kathy Vizas, Co-Founder of TogetHER, a new partnership focused on ending cervical cancer. “TogetHER is in a position to join the right funders with these really good organizations on the ground and help them to scale their programs, so that they are reaching not just a community, but a whole country.”
Close to 90 percent of cervical cancer deaths globally occur in less-developed countries. High-income countries demonstrate what is possible when adequate resources are available: Australia, for example, could be the first country to eliminate cervical cancer. According to Dr. Suzanne Garland from the Royal Women’s Hospital in Melbourne, the number of new cases is projected to drop to “just a few” over the next 40 years, after implementation of a free HPV vaccine program in schools, in combination with an HPV screening test.
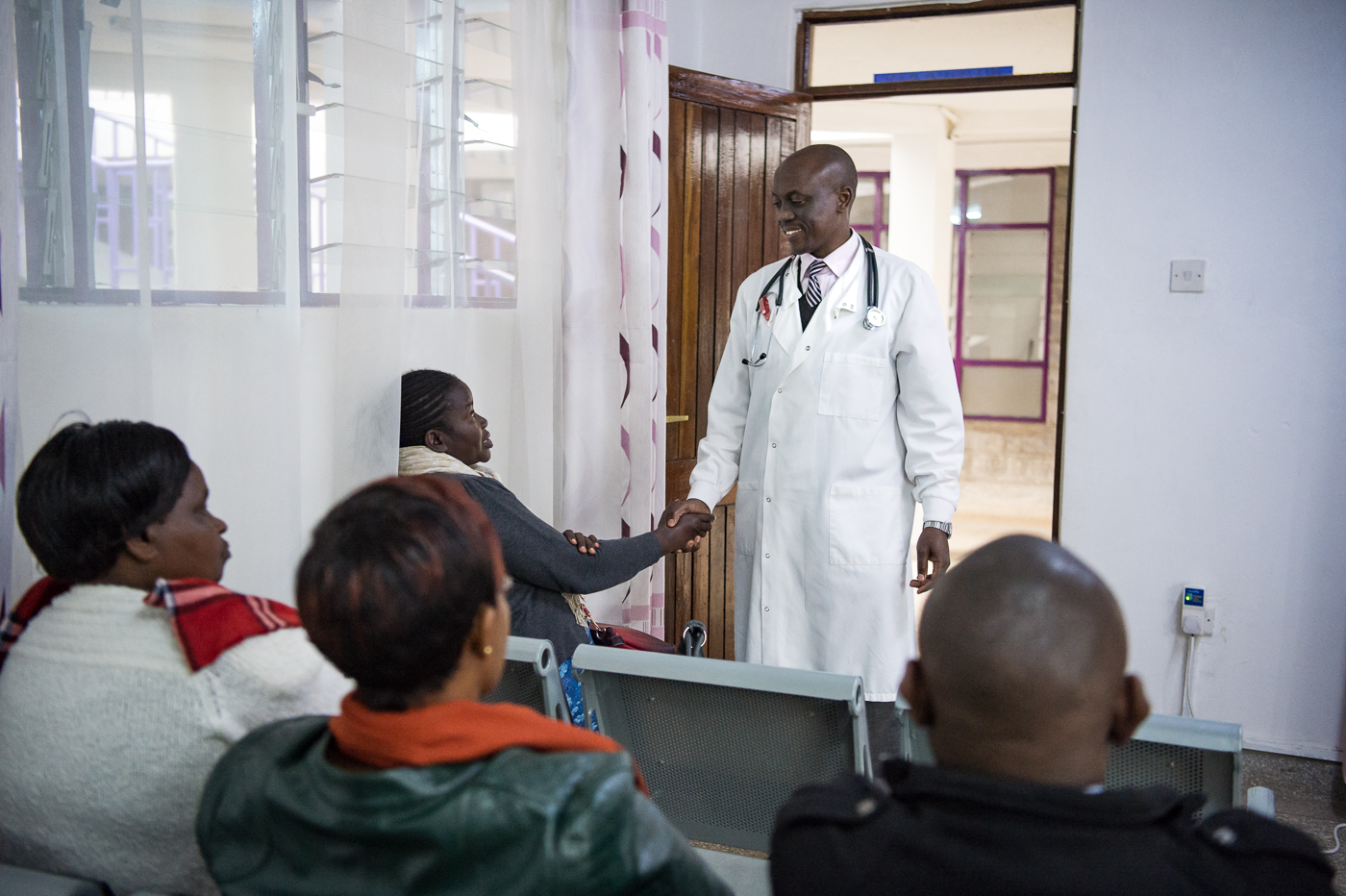
- Dr. Maranga walks through his private clinic, which also provides free care for women with advanced stages of cervical cancer who cannot afford the treatment.
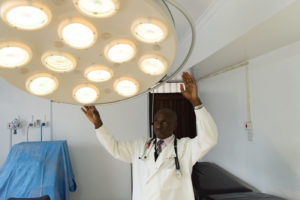
- Dr. Maranga prepares to perform a hysterectomy on one of his patients.
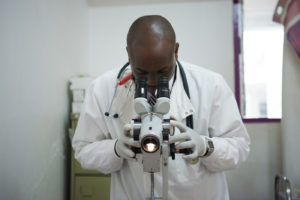
- Dr. Maranga evaluates a patient’s cervix through a colposcope.
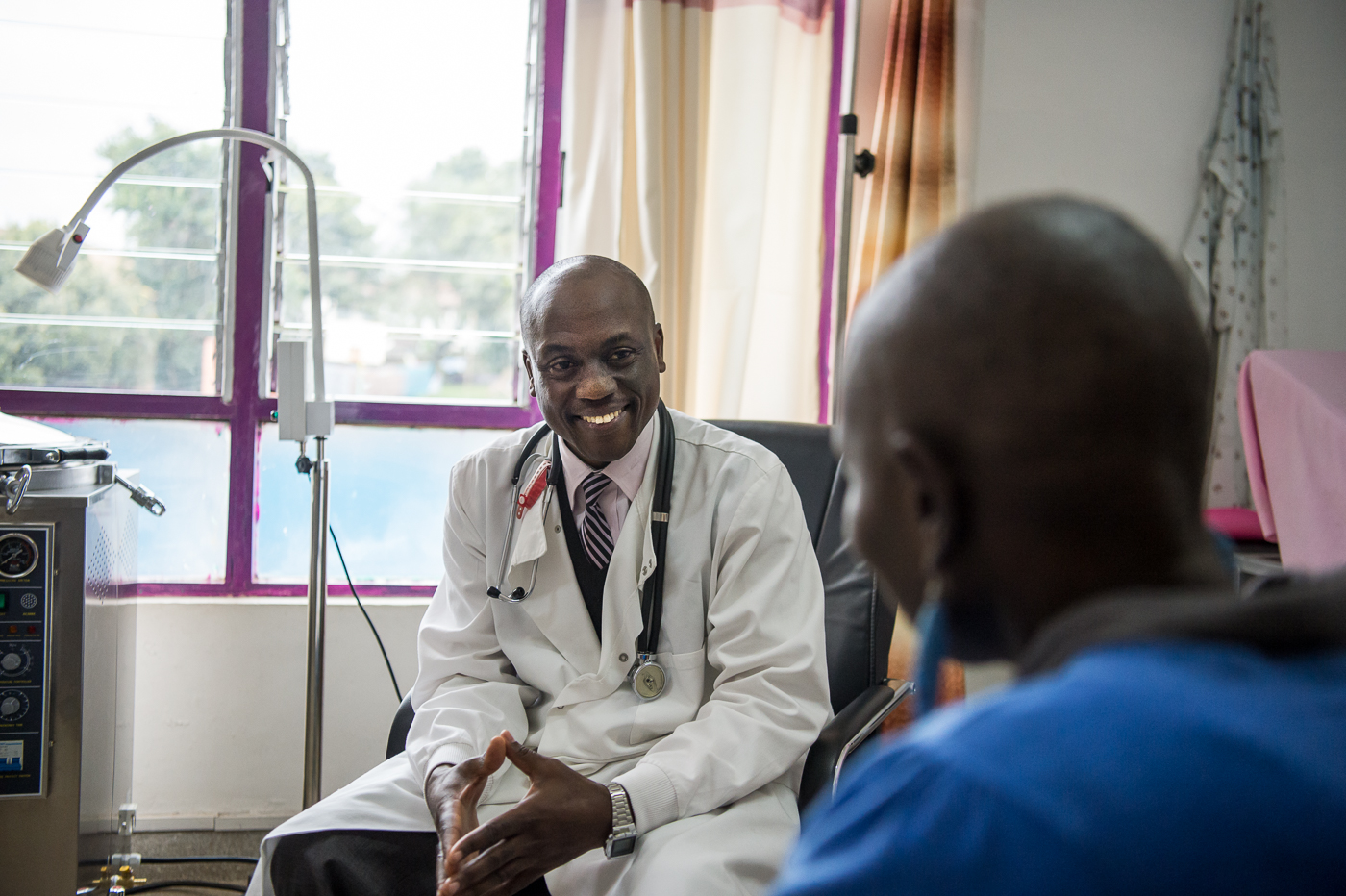
- During a consultation, Dr. Maranga takes notes on his patient’s condition and follow up.
There is a need for a concerted, well financed and united global push to ensure women who are vulnerable to cervical cancer are not left behind in countries with far fewer resources, like Kenya. By scaling up access to the tools already available, it is possible to end cervical cancer deaths around the world.
Dr. Maranga provided a practical point of view on the steps to stop cervical cancer in his country. He spoke about increasing screenings, so that cervical cancer can be prevented, and women diagnosed with cancer can be treated early. And he noted, “We need to increase vaccination around the country, and at the same time we need to look at the treatment, making it more accessible and affordable.”
But the first step, he said, was simply raising awareness, because too many women do not realize that they are at risk, or know how to protect themselves. “Women and families and communities need to be very much aware of cervical cancer, so awareness is one of the biggest things.”